This biological pacemaker is all muscle
Researchers have used gene therapy to reprogram cells in the heart
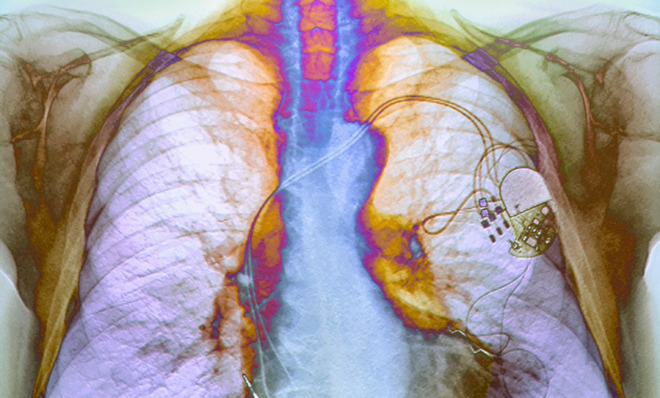

Scientists working in pigs have used gene therapy to convert a small area of heart muscle into a specialized group of cells that can initiate a heartbeat, essentially creating a biological pacemaker.
Normally, the heartbeats of pigs, as in humans, originate from a specialized clump of cells called the sinoatrial node. Sometimes diseases of the heart's electrical system can compromise this node and cause abnormal heart rhythms, which are often treated by implanting an electronic pacemaker to regulate the heartbeat. Some 300,000 electronic pacemakers are implanted in the U.S. alone every year. But there are some patients with abnormal heart rates that can't have a pacemaker implanted, such as unborn fetuses. And sometimes patients develop infections from the device, and need to go without a pacemaker for a limited time while they're being treated.
Now, a team of researchers from the Cedars-Sinai Heart Institute and Taipei Veterans General Hospital in Taiwan say they've found a new solution for these patients with a technique that uses gene therapy to reprogram cells of the heart. They reported their results Wednesday in the journal Science Translational Medicine.
The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
(More from World Science Festival: The science of family ties: 'It's all relatives')
The injection of a single gene, TBX18, into a peppercorn-sized patch of heart muscle, "converts ordinary heart cells to specialized sinoatrial cells," Cedars-Sinai researcher and paper co-author Eduardo Marban told reporters on a conference call Tuesday. "We create a new sinoatrial node in an area of the heart that normally just spreads the impulse."
TBX18 is a type of gene called a transcription factor, meaning that it regulates the expression of other genes in a cell's DNA. It appears to play an important role in the embryonic development of the heart.
In these experiments, the researchers deliver TBX18 to pig heart muscle cells with an adenovirus acting as courier. The virus is modified to carry TBX18; when it infects the pig cells, the viral DNA is inserted into the cell's nucleus, along with the TBX18 code. If all goes well, the cells should incorporate the gene of interest and start making the corresponding protein. In this case, the scientists saw biological pacemaker activity in treated pigs within 48 hours.
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
It may be several years before the biological pacemaker can be studied in humans, but if it proves effective and safe, the procedure would be fairly easy for doctors to perform using their existing facilities. There would be no open-heart surgery required, and little in the way of follow-up, since the biological pacemaker regulates itself. And in this study, the gene was delivered to the pigs' hearts with a catheter that's already in use in human studies.
(More from World Science Festival: Watch pioneering geneticist Mary-Claire King at The Moth)
"We wanted to use clinically realistic, minimally invasive approaches," coauthor Yu-Feng Hu, a researcher at the Cedars-Sinai Heart Institute, told reporters on a conference call.
More work will need to be done to confirm the treatment's usefulness and study its side effects. This particular study involved just 12 pigs, monitored for 14 days, and the researchers noted that treated pigs did have a higher average heart rate than the control animals. And while the vast majority of the virus (98.2 percent) overwhelmingly stayed put at the injection site, the researchers did find some small traces of adenovirus in the pigs' spleens and lungs two weeks after injection — although, the researchers noted in the paper, there was no sign that the viral DNA was being expressed in those organs.
Gene therapy holds great promise, but still carries risks. The use of viral vectors can cause problems when a patient's immune system overreacts, as was the case with Jesse Gelsinger, a patient who died during one of the first major clinical trials of gene therapy back in 1999. The field subsequently stalled in the U.S., with no treatments available outside of a clinical trial, but is experiencing a recent renaissance, particularly in the field of fertility (explored in depth at the 2014 World Science Festival program "Designer Genes: Fashioning Our Biological Future").
If the biological pacemaker pans out, it may offer a model for a host of other uses for gene therapy and cellular reprogramming. Cochlear cells in the ear could be reprogrammed to turn into hair cells to restore hearing in the hearing impaired, for example.
(More from World Science Festival: The long shadow of the Manhattan Project)
The biological pacemaker concept "is very exciting because it shows how gene therapies are not limited to curing rare genetic deficiencies, but can even impact diseases in genetically normal people which would typically be treated by mechanical devices," Harvard University geneticist George Church, who was not involved in the current study, wrote in an email. "It is remarkable that at this early stage a single gene delivery can provide enough support for both heart rate and physical activity even without any backup electronic pacing."
