The 'spray-on skin' that heals wounds
A new sprayable solution of recycled skin and blood-clotting proteins could revolutionize how we treat hard-to-cure wounds
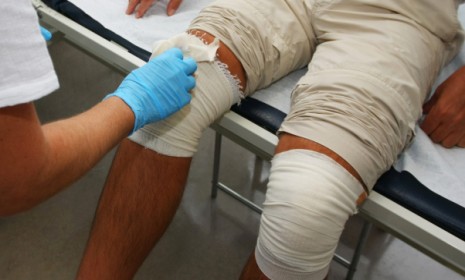
Healthpoint Biotherapeutics, a company out of Fort Worth, has successfully tested a spray-on treatment that promises to help wounds heal faster and without the need of skin grafts. Dr. Robert Kirsner at the University of Miami and his colleagues tested the "spray-on skin" on 228 patients with leg ulcers, or open wounds that are notoriously hard to heal. The result was "superior healing and a faster time frame than anything else we've seen in the treatment of venous leg ulcers," Kirsner tells MedNews Today. The study, published in the prestigious British medical journal The Lancet, is preliminary, but outside experts are impressed. Here's a look at the possible future of wound therapy:
What's the skin spray made of?
Healthpoint's spray, currently sporting the decidedly un-mellifluous name HP802-247, is made of donated skin cells (keratinocytes) and an anti-clotting agent (fibroblasts). The two substances are believed to work together to speed up healing and stimulate the body's production of new skin to cover the wound. The standard treatment for leg ulcers is a compression bandage, which heals up to 75 percent of the lesions within six months.
The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
Does this study prove that the skin-in-a-bottle works?
No. But the point was to make sure the spray was safe and determine the optimal dose, which turned out to be the lowest one: Spraying patients every 14 days. The results exceeded expectations: After three months, 70 percent of the patients receiving both the optimal dose of the spray-on skin treatment and traditional compression had completely healed versus 46 percent of the control group, which was using a placebo spray and compression bandages. Patients sprayed with the solution every 14 days also saw their wounds close 21 days before the control group, in 50 days versus 71 days. The size of the wound started shrinking almost immediately after spraying started with the skin solution.
What's next for spray-on skin?
Kirsner is already enrolling people in the U.S. and Europe for a Phase III clinical trial, to see if the treatment is feasible. Part of the issue is cost — it's expensive to turn the donated neonatal foreskin (circumcision trimmings) and blood-clotting proteins into a usable spray. In an accompanying commentary, Matthias Augustin at the University Medical Center in Hamburg, Germany, said the price tag may make more sense over the long term, especially for hard-to-treat wounds like leg ulcers: "The temporary higher costs for additional cell and tissue-engineered therapy can be justified as an investment in improved healing."
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
Is there a downside?
Besides cost, there's the risk of false hope for those suffering from painful leg ulcers, says leg ulcer theorist Irene Anderson at Britain's University of Hertfordshire. "Leg ulcers are becoming increasingly complex, and when using the range of treatments available there needs to be clear evidence that there will be a beneficial effect to ensure cost effectiveness and to make sure that patients are not given false expectations of a cure."
Sources: BBC, Daily Mail, Engadget, Examiner.com, MedPage Today
