The science behind lab-grown blood
Development of ‘absolute game changer’ could help those with sickle cell and other conditions
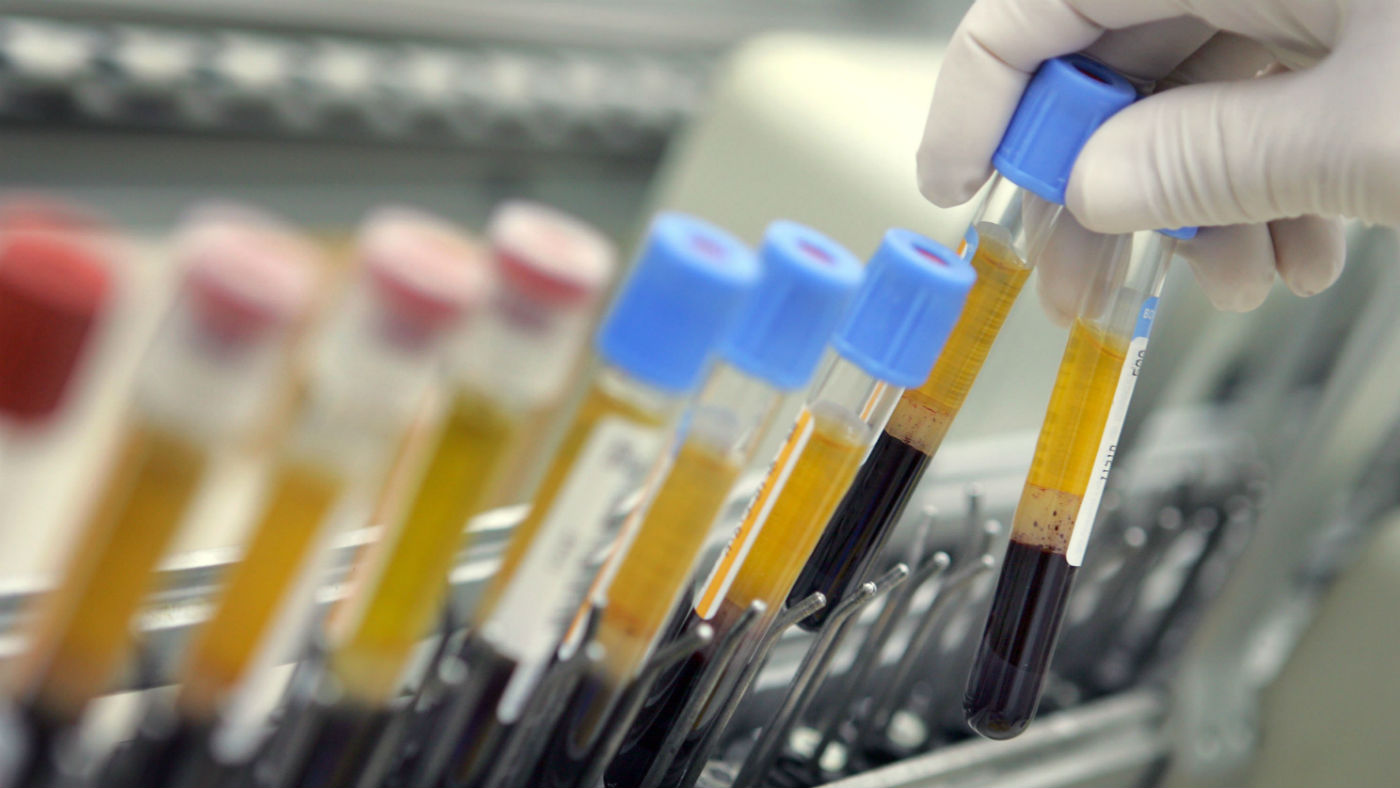
Laboratory-grown red blood cells have been transfused into people in a world-first clinical trial.
In a development that “could significantly improve treatment for people with blood disorders and rare blood types”, small amounts of lab-grown red blood cells were tested to see how they perform inside the body, said CNBC.
The two people transfused with the lab-grown red cells were closely monitored and remain “well and healthy” and have suffered no side effects, said the University of Cambridge. This is the first time that red blood cells grown in a laboratory have been given to another person as part of a trial into blood transfusion.
The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
How is blood grown in a lab?
The three-week process begins when scientists take a normal donation of a pint of blood and use magnetic beads to “fish out” flexible stem cells that are capable of becoming a red blood cell, said the BBC.
These stem cells were encouraged to grow in large numbers in the lab and are guided to become red blood cells. They were transfused in quantities of around 5-10ml – about one to two teaspoons – into the volunteers.
What are the benefits?
The aim of the trial is to manufacture vital, but ultra-rare, blood groups that are hard to get hold of. The University of Bristol’s Prof Ashley Toye said some blood groups were “really, really rare” and there “might only be 10 people in the country” able to donate these.
However, if they were produced in bulk in labs, red blood cells can be “tuned to have whichever blood type is needed”, said New Atlas. This addresses the two challenges the blood donation system faces: that demand “far outstrips supply” and the “extra hassle” of “matching blood types”.
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
Therefore, the development “could be an absolute game changer for increasing supplies of previously ultra-rare blood types”, agreed Popular Science, “and may even one day enable smaller and less frequent transfusions”.
If the manufactured cells prove to last longer in the body and patients require less transfusion, it would bring down the iron overload from frequent blood transfusions, which can lead to “serious complications”, said The Independent.
What are the challenges?
Harvested stem cells “eventually exhaust themselves”, said the BBC, which limits the amount of blood that can be grown. Therefore, “it will take more research to produce the volumes that would be needed clinically,” the broadcaster added.
Then there is the question of cost. While the average blood donation costs the NHS around £130, growing blood will cost significantly more. However, a spokesperson from NHS Blood and Transplant told CNBC, “if the trial is successful and the research works, then it could be introduced at scale in future years, meaning that costs would fall”.
What do experts say?
John James OBE, Chief Executive of the Sickle Cell Society, said the research “offers real hope for those difficult to transfuse sickle cell patients who have developed antibodies against most donor blood types” but added that “the NHS still needs 250 blood donations every day to treat people with sickle cell and the figure is rising”.
Dr Farrukh Shah, Medical Director of Transfusion for NHS Blood and Transplant, agreed that “the need for normal blood donations to provide the vast majority of blood will remain” but added that “the potential for this work to benefit hard-to-transfuse patients is very significant”.
Chas Newkey-Burden has been part of The Week Digital team for more than a decade and a journalist for 25 years, starting out on the irreverent football weekly 90 Minutes, before moving to lifestyle magazines Loaded and Attitude. He was a columnist for The Big Issue and landed a world exclusive with David Beckham that became the weekly magazine’s bestselling issue. He now writes regularly for The Guardian, The Telegraph, The Independent, Metro, FourFourTwo and the i new site. He is also the author of a number of non-fiction books.
