Living with lupus
"I was sick. I didn't want to people to see me. I didn't want to see myself. I didn't want to live. It was more than I could take."


As a child, Sandra Bettinger was never allowed to use her lupus as an excuse for anything.
On school mornings, if Bettinger was feeling fatigued or simply didn't want to deal with bullying classmates mocking her swollen body, she would desperately devise a plan to stay home. Standing in front of the air conditioner, shivering, she would hope for little white polyps to form on her tonsils or some other physical signs of her illness to appear.
"Look Ma," Bettinger would say in their absence, hopeful she could pull off the ruse. "I'm sick."
The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
But before her mother could answer, her father's deep voice would boom from her parent's bedroom: "You are going to school."
Throughout her childhood, Bettinger says her father challenged her whenever she claimed to feel sick. He learned to identify when her confessed fevers were real and when they were not.
"It's all in your head," he'd tell her when he suspected she was lying.
Fearing her symptoms would be challenged by her father, Bettinger began to keep them to herself. Over time, she started keeping her symptoms hidden from everyone.
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
Bettinger's lupus became a dangerous secret.

Systemic lupus erythematosus is an autoimmune disease characterized by an overactive immune system that mistakenly attacks healthy tissue and organs in the body, including the skin, joints, kidneys, lungs, brain, and heart. This causes an unpredictable range of symptoms such as fatigue, rashes, joint inflammation, muscle pain, or organ failure, some of which can lead to death.
The exact cause of lupus is still unknown, and in most cases, the afflicted have never heard of the disease before their diagnosis. Research indicates patients may have a genetic predisposition to it that may be activated by environmental factors, such as stress, infections, certain medications, or sunlight. While Lupus can strike anyone, 90 percent of its victims are women and most of the initial diagnoses occur between the ages of 15 and 44. Bettinger was first diagnosed with lupus at the age of 10, after she developed a rash across her face, known as a "butterfly rash."
(More from Narratively: Crooked lines)
As she got older, Bettinger went to great lengths to hide her symptoms. In graduate school, she sometimes wore long white cotton gloves, long sleeves, and a hat.
In fact, her attempt to camouflage her puffy limbs on a study-abroad trip in England led to a severe flare-up of the disease that went untreated for weeks. Her whole body was swollen and she was embarrassed by her appearance. By the time she was on her flight home to New York, she couldn't conceal her symptoms any longer and knew she was severely ill. In great pain, she was rushed to the hospital upon landing.
Bettinger was issued a high dose of Prednisone, an immunosuppressant steroid. She recovered, but something had changed. Even though she was living at home in New York surrounded by family, she felt severely depressed. Her days were spent juggling prescription medications and handling hours-long doctor's appointments. She felt alone, and trapped indoors where the sun couldn't hurt her.
"I was like a zombie, the walking dead," Bettinger recently said in a raspy voice as she stubbed out a cigarette on her kitchen counter. "I had lost that one thing, [hope], that held me together, that one fiber the kept me from going over the edge, of wanting to end it. I was sick. I didn't want to people to see me. I didn't want to see myself. I didn't want to live. It was more than I could take; all I could think was, I can't live, I can't. I'm awake all day looking at the ceiling. I can't sleep at night. It hurts to live."
Shortly after completing graduate school at NYU in 1982, Bettinger tried to commit suicide in her family home. She ended up in the voluntary psychiatric ward at Booth Memorial Hospital in Queens.
(More from Narratively: The burn of the beautiful blowout)
According to the U.S. Department of Health and Human Services, 1.5 million Americans suffer from lupus, with 16,000 more developing the illness each year. Lupus is more common than leukemia, muscular dystrophy, cerebral palsy, multiple sclerosis, and cystic fibrosis, and there is no cure. However, this painful, chronic autoimmune disease remains obscure to the public. The Lupus Foundation of America states that 61 percent of Americans either have never heard of it or know little more than the name of the illness.
AIDS and lupus are both autoimmune diseases, but they differ because AIDS causes the immune system to be underactive, whereas lupus causes it to be overactive. With lupus, the immune system attacks the body. (Lupus also differs from AIDS in that it isn't spread contagiously by a blood-borne virus, although its exact cause remains unknown.)
"It's like friendly fire within the body," explains Dawn Isherwood, a health educator for the Lupus Foundation of America. "Rather than going after a virus or bacteria, the immune system is going after the wrong thing."
Which organ is attacked varies with each patient. Bettinger's eyes and joints have been particularly affected.
Experts have called lupus "the great imitator" and "the trash-bin of autoimmune diseases" because its symptoms are so vague and common to many other illnesses. Not all symptoms and identifiers are present at any given time.
"Often times, as lupus is starting to develop, it plays peek-a-boo," says Isherwood. "It's like looking at one of those old Polaroid pictures. Until that picture becomes 80 to 85 percent developed, there may be some ambiguities as to what it is."
Today, Bettinger is resigned to her illness. With the help of the psychiatric treatment she received at Booth Memorial, she slowly recovered from her bout of clinical depression. But her physical symptoms persist. Lately she has been battling an inflammation of the skin around her eye.
"Life goes on," says Bettinger, who lives alone. Her income is restricted to disability checks. "I don't have a husband or a child, so I still sometimes battle isolation, but I try to reach out in support groups."
(More from Narratively: The hair down there)
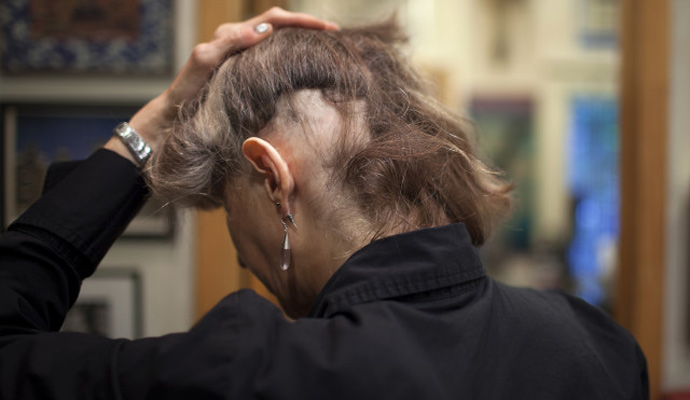
It is common for sufferers of chronic illness to experience depression, according to a study published last year in the journal Social Work in Health Care, so support from friends, family and professionals is critical. However, oftentimes the supporters do not understand the illness. Not only have many never heard of lupus, but 42 percent of people in the United States do not believe lupus is disabling and fail to realize its ramifications. Many researchers and social workers believe this is because lupus is relatively invisible. Rashes tend to go away with medication, hair loss can easily be covered up, and weight gain isn't always obvious. Symptoms like fatigue are also vague and difficult to distinguish from normal fatigue.
"People don't look sick," explains Jessica Rowshandel, director of social services at the S.L.E. Lupus Foundation, and a frequent leader of the organization's Manhattan support group chapter. "If [patients] came in a wheelchair and looked really pale and their face was sunken in, maybe they would get a little bit more support. Family and friends, when they think of joint pain or fatigue, they think it means 'tired,' so they don't understand why [the patient] can't move, go to work or do the dishes."
For this reason, Rowshandel advises patients to describe their symptoms and extreme exhaustion precisely and in a way people can understand. For example, "It feels like the flu," or "It feel like I just ran a marathon," or "It feels like two tons of metal are on top of my body."
Read the rest of this story at Narratively.
Narratively is an online magazine devoted to original, in-depth and untold stories. Each week, Narratively explores a different theme and publishes just one story a day. It was one of TIME's 50 Best Websites of 2013.
