Is it time for doctors to ditch the white coat?
The traditional uniform is causing more problems than you think
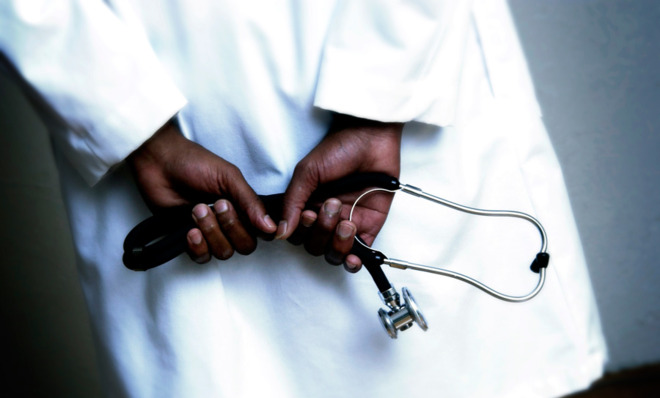
Anyone who has considered medicine as a career imagines walking into a white, clean exam room with the power to comfort and heal the sick. To add to this angelic fantasy, we do not forget to imagine ourselves wearing a freshly laundered white coat bearing what only many years of arduous education and sleepless nights can provide: First name, last name, M.D.
The white coat is a badge of perseverance, intelligence, empowerment, and authority — for new interns, a reassurance that they have what it takes to take care of the life of another. But this Victorian symbol of purity and sanitation may soon go the way of the lobotomy.
I recently returned from an interview at Mayo Clinic, where I was surprised to see so many business suits. As one of the world's meccas for medicine and health care, I expected a place that resembled, well, a hospital. Instead I encountered what appeared to be a fancy hotel with a curiously large number of wheelchairs.
The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
The rationale behind the white coat restriction makes sense given Mayo's dedication to providing the best for patient care and comfort. The organization's philosophy: The white coat builds a barrier between patient and physician, increasing the chances for the patient to feel anxious.
And Mayo patients seem to like it. Surveys have found that patients felt most comfortable when physicians wore scrubs, followed by semi-formal/business attire, then followed last by white coats. In order to maintain its high standards of professionalism, Mayo went with the suit and eschewed the white coat. (The only ones who can wear white coats in public are those in scrubs coming from or going to the OR.)
In a separate 2005 report published in the British Medical Journal, researchers found that patients preferred doctors wearing semiformal attire — defined as dark pants and long-sleeved shirt with a tie for men, and dark-colored skirts or pants with a blouse for women. Those ensembles beat out the white coat, formal wear, and casual attire.
Mayo is not alone in recognizing the symbolic power of the white coat. As Jean-Phillip Okhovat, a UCLA medical student, puts it, "I think the white coat creates an immediate sense of hierarchy. Not wearing a white coat makes it less intimidating for the parent and child."
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
In psychiatry, the white coat can not only add to this patient-physician barrier, but also become a target of aggression for patients with a history of troubled visits to the doctor. Yang Yu, a University of California, Irvine, medical student, recalls, "Mentally ill patients can perceive the white coat as a threat. There have been instances of people in white coats who were attacked."
Inevitably, when the topic of white coats comes up, the issue of spreading infections is never far away. Even as someone who works in health care, the white coat can sometimes make me cringe. I have no idea how many hundreds of patients that coat rubbed up against, and sometimes I can tell that the coat has not been washed in weeks. The gloves get changed, the paper on the examination bed gets rolled out, and copious amounts of hand sanitizer are used, but none of that may matter if the biggest culprit is right on the doctor's clothes.
In one study, researchers found that doctor's white coats were contaminated with all kinds of bacteria, including Staphylococci resistant to penicillin, erythromycin, and clindamycin. The worst areas were the sides of the white coat, the cuffs, collars, and pockets.
The National Health Service in the U.K. has already banned the use of long-sleeved white coats, and instead adopted a "bare below the elbows" rule to reduce unnecessary infections. The NHS also requires that doctors leave their uniforms at the workplace, where it is regularly laundered to reduce cross-contamination. This policy has already shown a marked reduction in infections. (I should mention, however, that despite evidence showing that white coats harbor bacteria, many professionals remain unconvinced that this makes a difference in terms of nosocomial infections.)
Every July and August of each year, recently admitted medical students don fresh white coats to symbolize the beginnings of this arduous yet rewarding journey toward becoming a physician. But the tone is changing as physicians continuously ask themselves how best to serve their patients. As Don Berwick, a Harvard Medical School professor and former Administrator of the Center for Medicare and Medicaid Services, put it at the commencement for the Yale School of Medicine in 2010:
Those who suffer need you to be something more than a doctor; they need you to be a healer. And to become a healer, you must do something even more difficult than putting your white coat on. You must take your white coat off.
When you take off that white coat in the sacred presence of those for whom you will care — in the sacred presence of people just like you — when you take off that white coat, and tower not over them, but join those you serve, you become a healer in the world of fear and fragmentation.
-
 Gavin Newsom and Dr. Oz feud over fraud allegations
Gavin Newsom and Dr. Oz feud over fraud allegationsIn the Spotlight Newsom called Oz’s behavior ‘baseless and racist’
-
 ‘Admin night’: the TikTok trend turning paperwork into a party
‘Admin night’: the TikTok trend turning paperwork into a partyThe Explainer Grab your friends and make a night of tackling the most boring tasks
-
 Find art, beautiful parks and bright pink soup in Vilnius
Find art, beautiful parks and bright pink soup in VilniusThe Week Recommends The city offers the best of a European capital