The COVID 'long-haulers'
Even after supposedly recovering, thousands of Americans are suffering persistent and even disabling symptoms
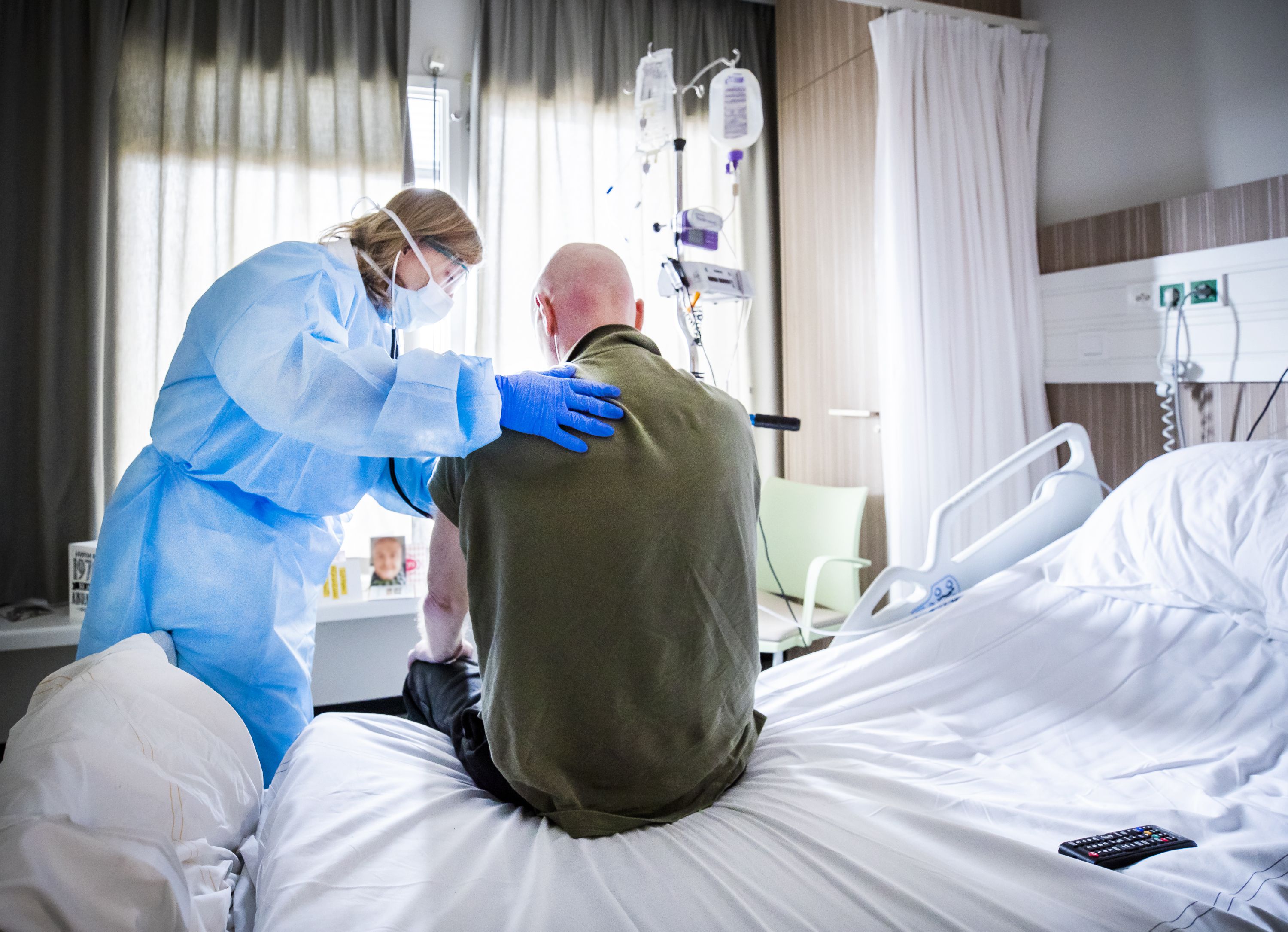
Even after supposedly recovering, thousands of Americans are suffering persistent and even disabling symptoms. Here's everything you need to know:
What is "long-haul" COVID?
It's a persistent and wide-ranging set of symptoms that follow a coronavirus infection. Nearly 100 kinds of lingering symptoms and physical damage have been catalogued, including scarred lungs, chronic heart damage, severe headaches, kidney failure, bulging veins, hand tremors, debilitating fatigue, fever, nausea, stomach problems, hair loss, sensitivity to light and sound, blurry vision, loss of taste and smell, short-term memory loss, and a brain fog so dense it can be difficult to write even a simple email. New York City resident Deborah Copaken, 54, was diagnosed with COVID-19 in March and still suffers from shortness of breath and the repeated and sudden onset of a rapid heartbeat so severe that she must lie down in order to avoid passing out. "A few weeks ago," she said, "I stood up to make a smoothie and my heart rate zoomed from lying-in-a-hammock to booming-bass-drum." David Putrino, a neuroscientist at Mount Sinai Hospital who has treated many long-haulers, says his patients struggle with a bewildering array of maladies. "It's like every day, you reach your hand into a bucket of symptoms, throw some on the table, and say, 'This is you for today.'"
The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
What is causing these symptoms?
Research indicates that the coronavirus is far more than a classic respiratory illness and can attack organs throughout the body. The virus binds itself to cells using a protein on the surface of the cells called ACE2. These ACE2 receptors are found inside blood vessels; on olfactory bulbs that provide a sense of smell; on kidneys; in the gastrointestinal tract; and, according to new research, in the brain. The immune system's overreaction to the viral invasion can compound the damage, with severe inflammation and blood clots impairing the heart, lungs, and other organs. "It's amazing how many different ways it affects the body," said Thomas McGinn, deputy physician in chief at Northwell Health. If the virus penetrates the brain, a new study found, it replicates and starves nearby cells of oxygen, diminishing the number of synapses — connections between neurons. "We don't know yet if that is reversible or not," said Dr. Alysson Muotri, a neuroscientist at the University of California, San Diego. These findings may explain why 40 to 60 percent of hospitalized COVID-19 patients experience psychiatric and neurological symptoms, including brain fog, delirium, crippling headaches, anxiety, and depression.
Are long-haulers generally old?
Unlike the majority of people whom COVID kills, many long-haulers are relatively young: Putrino's survey of 1,400 patients found they are mostly female and have an average age of 44. Some were previously quite healthy and fit. Isabela Pauer, for example, is 22 and used to work out four to five times a week. She developed COVID symptoms six months ago in Barcelona and today labors to brush her teeth. "My whole body feels, like, very weighted down," said the Cleveland-area resident. "I'm almost dragging myself around places." Like many long-haulers, she faced strong skepticism from doctors, who doubted that she was really sick. "I ended up like just kind of losing faith in getting any help at all," she said.
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
How many long-haulers are there?
Probably millions worldwide. A study in Italy found that 87 percent of COVID patients who were hospitalized still had symptoms two months after their release. A British study followed up with COVID patients eight to 12 weeks after hospitalization and found 74 percent still had "persistent symptoms," particularly fatigue and shortness of breath. In Germany, researchers found 78 percent of patients, including some who had recovered at home, suffered from heart abnormalities two to three months after their recovery. Meanwhile, researchers at the Centers for Disease Control and Prevention tracked 270 COVID patients who were not hospitalized and found that 95 — more than a third — hadn't fully gotten better within three weeks. The U.S. has had about 6.5 million confirmed cases, so the math points to hundreds of thousands and perhaps millions of long-haulers.
Are all cases equal?
No, there is a wide variation in severity. In milder cases, a handful of symptoms inexplicably come and go for months. In more severe cases, like Chimére Smith's, it becomes impossible to work. Smith, 38, a middle-school English teacher in Baltimore, has had COVID symptoms since March, including severe stomach problems and headaches, and has been to the emergency room a dozen times. Once highly verbal, she struggles with a chronic mental fog that makes it difficult for her to remember words or speak in complex sentences. "Who in the world would want to live like this?" Smith said. "I wanted to jump out of my own body." Hannah Wei, 30, an Ottawa-based product designer, gradually overcame her neurological symptoms but not the scarred lungs that have diminished her ability to exercise or even walk up a flight of stairs. "Will I be living with this lasting damage?" she asked. "Or will it eventually go away? I don't have the answers, and no one can tell me."
Sick, but never diagnosed
Many COVID long-haulers complain that they were denied tests early on in the pandemic because of shortages in diagnostic swabs and restrictions placed on who was eligible for scarce tests. Boston resident Lauren Nichols, 32, got sick in March but was denied a test by her doctor, who said at her age she was in no danger. She finally tested positive, and has suffered a debilitating array of symptoms consistent with those experienced by other long-haulers, including nausea, brain fog, insomnia, and shortness of breath. Complicating matters, said neuroscientist David Putrino, two-thirds of the 1,400 patients he studied did not test positive for COVID antibodies. Some, like Nichols, tested negative for antibodies even after testing positive for the virus itself. That can make it difficult for the afflicted to prove they have COVID and get paid time off from work or qualify for disability benefits. "Just because you're negative for antibodies," Putrino said, "doesn't mean you didn't have COVID-19."
This article was first published in the latest issue of The Week magazine. If you want to read more like it, you can try six risk-free issues of the magazine here.
