Shigellosis: The rise of an antibiotic-resistant stomach bug
Drug-resistant strains of the bacteria accounted for 5 percent of shigellosis infections in 2022

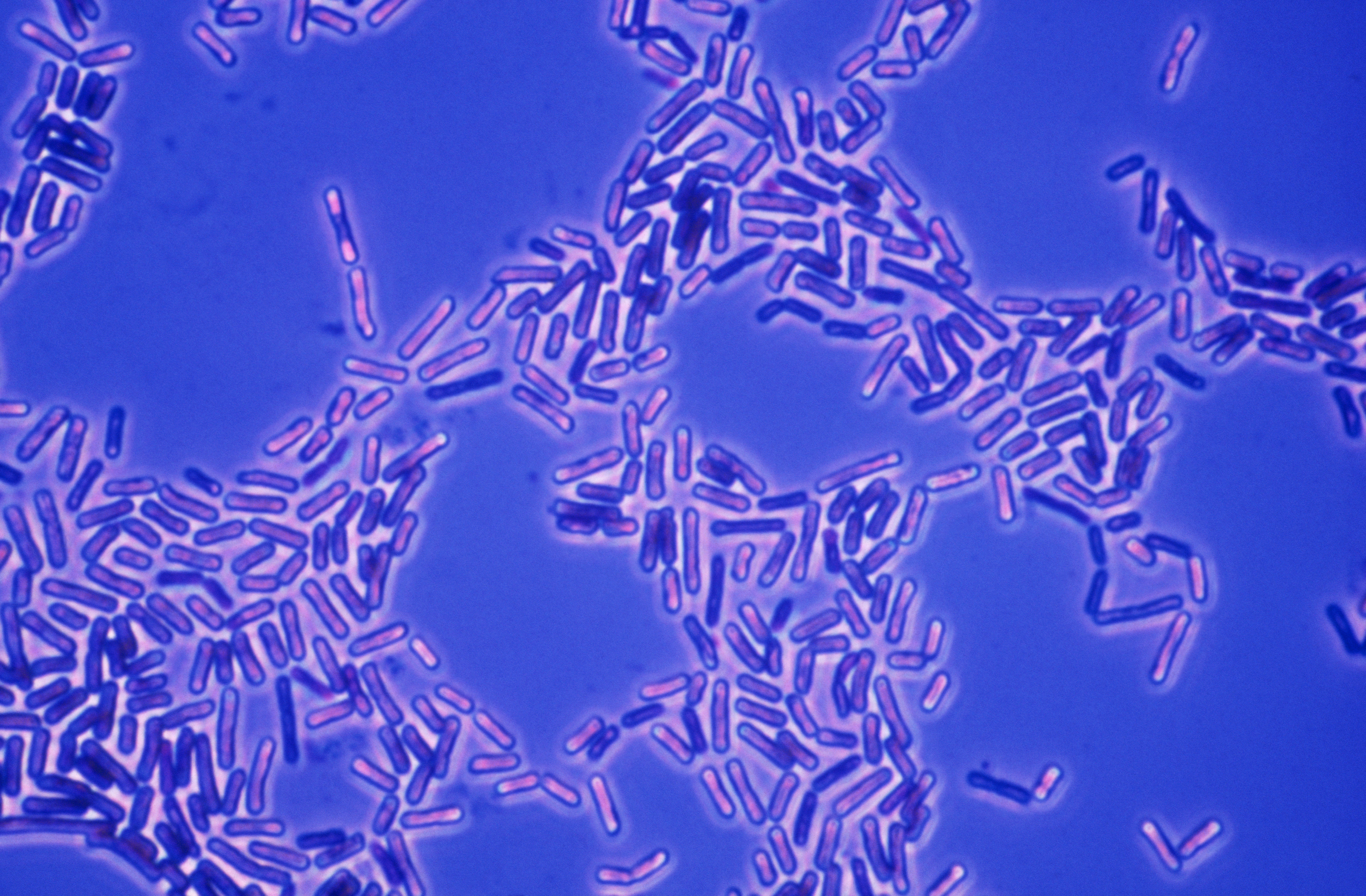
The Centers for Disease Control and Prevention issued a health alert in February saying it was monitoring a rise in drug-resistant Shigella infections, leaving doctors concerned over what this could mean for other bacteria. Here's everything you need to know:
What is Shigella?
Shigella is a bacteria that causes shigellosis, an intestinal infection. Symptoms of shigellosis include diarrhea, which can be bloody and last for more than three days, as well as fever and stomach pain. Shigella spreads easily, and is found in the feces of an infected person. Two common ways of getting infected include changing a diaper and then not washing your hands for long enough, or eating food prepared by someone who is infected.
Are Shigella infections common?
Every year, there are about 450,000 cases in the United States, with around 6,400 requiring hospitalization, the Centers for Disease Control and Prevention says. Most of the infections are in kids under 5.
The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
How are Shigella infections treated?
Most people recover after a few days of rest and drinking plenty of fluids. When an infection is severe enough to require further treatment or hospitalization, there are five antibiotics doctors usually turn to: azithromycin, ciprofloxacin, ceftriaxone, trimethoprimsulfamethoxazole, and ampicillin. Sometimes, Shigella strains won't respond to one or two of the antibiotics, but in the last few years, there has been an increase in cases where none of these antibiotics work.
The CDC said the first U.S. case of "extensively drug-resistant" Shigella was found in 2016, and by 2022, drug-resistant strains made up 5 percent of infections and were discovered in 29 states. These cases are primarily being reported among adults, particularly men who have sex with men, people who are experiencing homelessness, people with HIV, and international travelers, the CDC said.
There are other antibiotics that could work for Shigella, but have not yet been tested, so it is possible there are additional treatment options. As of now, "we have gone beyond the boundaries of what's been studied for Shigella," Dr. Louise Francois Watkins, a medical officer at the CDC, told The New York Times.
What causes antibiotic resistance in bacteria?
Bacteria are living organisms that evolve over time, and adapt to survive. The more antibiotics are used, "the more bacteria become resistant to them — that's a kind of inevitable evolutionary process," Stephen Baker, a professor of molecular microbiology at the University of Cambridge, told the Times. Mutations and gene transfers can allow bacteria to acquire drug resistance, and because Shigella is "particularly good at picking up new genes ... antibiotic resistance often emerges in Shigella before it does in other types of bacteria," the Times writes. That's concerning, Watkins said, because the resistance can spread from Shigella to other organisms, and "what we're seeing in Shigella now, this resistance is something that we could be seeing in other types of bacteria like E. Coli or salmonella in the future." Even if it isn't Shigella that is spreading resistance, this could possibly be "an early warning sign that these selective pressures are out there and that they're acting on other bacteria also," Watkins added.
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
How can you curb transmission of Shigella?
Wash your hands with soap and warm water for at least 20 seconds after using the bathroom or changing a diaper, before preparing food or eating, and prior to sexual activity. If you or your child is sick, stay at home, and see if your local health department has a policy on when kids can return to school or day care following a bout with a Shigella infection. For more ways to prevent Shigella infections, visit the CDC's website.
Catherine Garcia has worked as a senior writer at The Week since 2014. Her writing and reporting have appeared in Entertainment Weekly, The New York Times, Wirecutter, NBC News and "The Book of Jezebel," among others. She's a graduate of the University of Redlands and the Columbia University Graduate School of Journalism.

