Solving COVID: May 20, 2020
A potential vaccine shows early promise, doctors see signs of hope, and more
- 1. Potential coronavirus vaccine shows early promise
- 2. Doctors say growing 'toolbox' of coronavirus treatments gives them hope
- 3. Researchers find biomarkers that can predict COVID-19 patients' survival chances
- 4. Study suggests recovered patients' plasma is safe for treating COVID-19
- 5. Recovered coronavirus patients who tested positive again weren't infectious, Korean CDC finds
1. Potential coronavirus vaccine shows early promise
Massachusetts biotechnology company Moderna announced Monday that its potential COVID-19 vaccine showed promising early results in clinical trials. Eight patients developed antibodies at levels similar to those of people who recovered from the coronavirus, the company said. Critics caution that Moderna did not publish all the data, and say the announcement was too vague to draw any conclusions. "These are partial findings from a small, early-stage study," Boston Globe reports. "It's not known whether the dozens of other people in the study will have the same results." But Moderna described the interim data as "positive," with Chief Medical Officer Tal Zaks saying that the findings, though early, "substantiate our belief that mRNA-1273 has the potential to prevent COVID-19 disease." Moderna is moving into phase two of its clinical trials, having received approval from the Food and Drug Administration, and it says the third phase is expected to begin in the summer.
2. Doctors say growing 'toolbox' of coronavirus treatments gives them hope
In the early days of the coronavirus pandemic, doctors "were flying blind" as they tried to treat a disease with mysterious symptoms and very little research, Jose Pascual, a critical care doctor at the University of Pennsylvania Health System, told The Washington Post. But health-care workers everywhere have since "devised a toolbox, albeit a limited and imperfect one, of drugs and therapies" they believe are improving patients' chances of survival every day. Unexpected "curveballs" — like new symptoms and side effects — from the virus quickly became lessons. Hospitals started quickly measuring oxygen levels in any suspected coronavirus patients, and learned how to boost breathing support. They knew to look for effects in other parts of the body, not just the lungs. And after some once-promising drugs proved unhelpful, doctors have been able to rule them out in favor of more effective drugs. Of course, experimental approaches will have to be further researched through randomized clinical trials before they're approved for general use.
Subscribe to The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
3. Researchers find biomarkers that can predict COVID-19 patients' survival chances
Two COVID-19 studies released last week offer tools that might help hospitals better triage patients. Researchers in China reported in the journal Nature Machine Intelligence that an analysis of blood samples taken from 485 coronavirus patients in Wuhan discovered biomarkers that can predict whether a coronavirus patient will die within 10 days, with more than 90 percent accuracy, Business Insider reports. A computer model the researchers developed looks for high levels of the enzyme lactic dehydrogenase (LDH), linked to lung damage; lymphopenia, or low levels of infection-fighting white blood cells; and a rise in inflammation-signaling high-sensitivity C-reactive proteins (hs-CRP). "... This simple model can help to quickly prioritize patients, especially during a pandemic when limited health-care resources have to be allocated," the researchers said. A second paper published in the Journal of the American Medical Association found 10 biomarkers researchers said could predict a patient's risk. They turned risk predictors — high LDH levels and low levels of lymphocytes plus age, history of cancer, shortness of breath — into a coronavirus risk "calculator."
4. Study suggests recovered patients' plasma is safe for treating COVID-19
An experimental COVID-19 treatment known as convalescent plasma transfusions appears to be safe and could be a worthwhile treatment after it's studied more, a recently published study suggests. Researchers at the Mayo Clinic, Michigan State University, and Johns Hopkins University looked at 5,000 coronavirus patients around the country who received convalescent plasma transfusions from recovered patients. Less than 1 percent of the treated patients saw "serious adverse effects" after the transfusions, and there was a 14.9 percent mortality rate seven days after transfusions. Two-thirds of these patients were critically ill to begin with, so "the mortality rate does not appear excessive," the study said. While this study doesn't determine whether convalescent transfusions effectively treat coronavirus, it does suggest they are safe for wider research. The study will need to be peer reviewed and replicated in official medical journals before it can be considered an approved way of treating COVID-19.
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
Medrxiv The Wall Street Journal
5. Recovered coronavirus patients who tested positive again weren't infectious, Korean CDC finds
The Korean Centers for Disease Control and Prevention studied 285 COVID-19 survivors who initially recovered from the illness but then tested positive again. They found these patients' virus samples couldn't be grown in culture, suggesting the patients had indeed recovered and were actually shedding non-infectious or dead virus particles, rather than suffering from a lingering infection. South Korean health authorities — who have received praise for setting a global standard during the pandemic — will no longer consider COVID-19 patients infectious after they recover, and won't require additional tests after patients are discharged from their isolation period. That means those patients won't have to test negative before returning to work or school. Another positive sign from the findings is that almost all of the cases for which blood samples were taken showed antibodies against the virus, suggesting that people who were previously infected do indeed build up some form of protection.
-
 Trump uses tariffs to upend Brazil's domestic politics
Trump uses tariffs to upend Brazil's domestic politicsIN THE SPOTLIGHT By slapping a 50% tariff on Brazil for its criminal investigation into Bolsonaro, the Trump administration is brazenly putting its fingers on the scales of a key foreign election
-
 3 questions to ask when deciding whether to repair or replace your broken appliance
3 questions to ask when deciding whether to repair or replace your broken appliancethe explainer There may be merit to fixing what you already have, but sometimes buying new is even more cost-effective
-
 'Trump's authoritarian manipulation of language'
'Trump's authoritarian manipulation of language'Instant Opinion Vienna has become a 'convenient target for populists' | Opinion, comment and editorials of the day
-
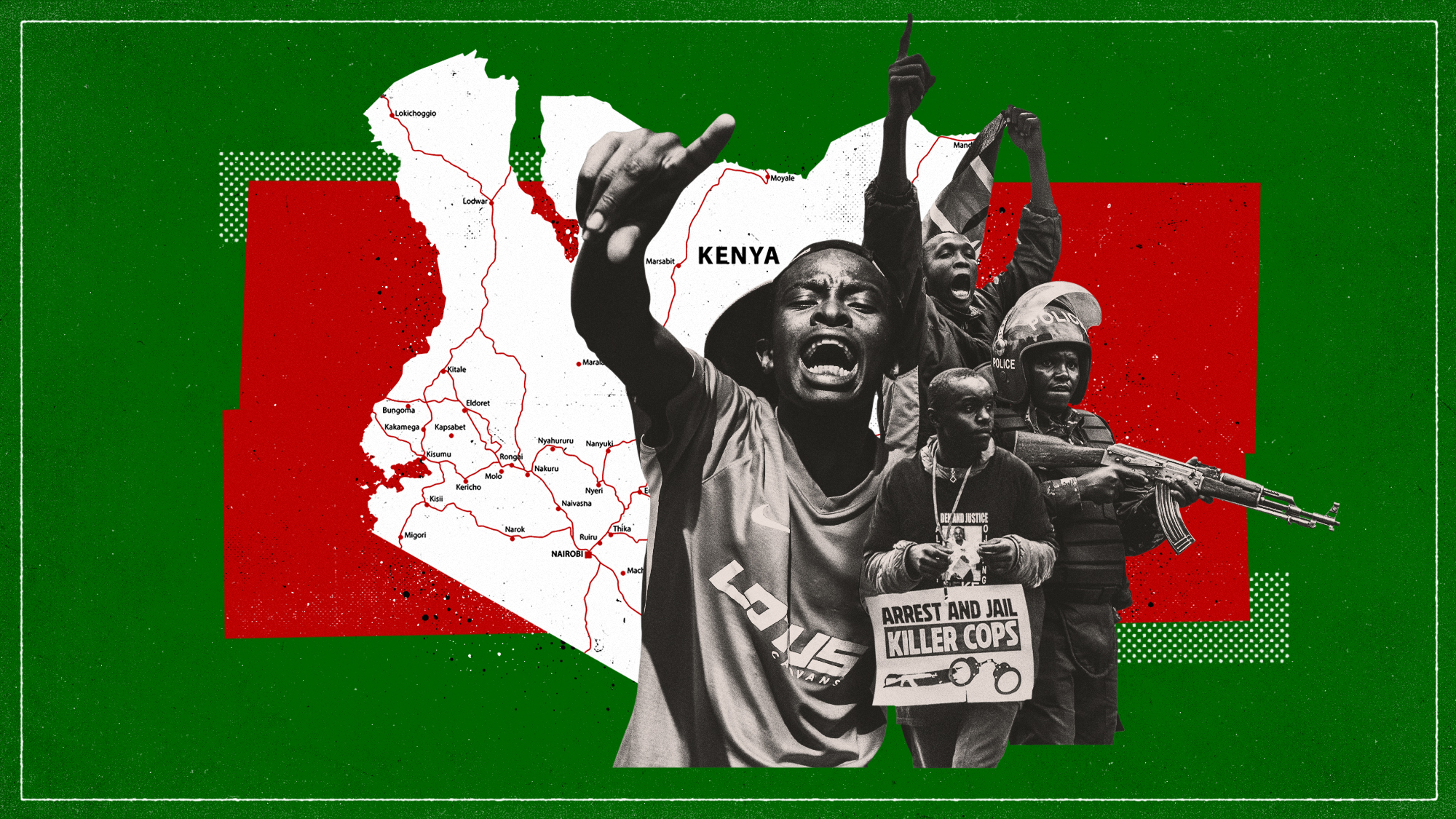 One year after mass protests, why are Kenyans taking to the streets again?
One year after mass protests, why are Kenyans taking to the streets again?today's big question More than 60 protesters died during demonstrations in 2024
-
 What happens if tensions between India and Pakistan boil over?
What happens if tensions between India and Pakistan boil over?TODAY'S BIG QUESTION As the two nuclear-armed neighbors rattle their sabers in the wake of a terrorist attack on the contested Kashmir region, experts worry that the worst might be yet to come
-
 Why Russia removed the Taliban's terrorist designation
Why Russia removed the Taliban's terrorist designationThe Explainer Russia had designated the Taliban as a terrorist group over 20 years ago
-
 Inside the Israel-Turkey geopolitical dance across Syria
Inside the Israel-Turkey geopolitical dance across SyriaTHE EXPLAINER As Syria struggles in the wake of the Assad regime's collapse, its neighbors are carefully coordinating to avoid potential military confrontations
-
 'Like a sound from hell': Serbia and sonic weapons
'Like a sound from hell': Serbia and sonic weaponsThe Explainer Half a million people sign petition alleging Serbian police used an illegal 'sound cannon' to disrupt anti-government protests
-
 The arrest of the Philippines' former president leaves the country's drug war in disarray
The arrest of the Philippines' former president leaves the country's drug war in disarrayIn the Spotlight Rodrigo Duterte was arrested by the ICC earlier this month
-
 Ukrainian election: who could replace Zelenskyy?
Ukrainian election: who could replace Zelenskyy?The Explainer Donald Trump's 'dictator' jibe raises pressure on Ukraine to the polls while the country is under martial law
-
 Why Serbian protesters set off smoke bombs in parliament
Why Serbian protesters set off smoke bombs in parliamentTHE EXPLAINER Ongoing anti-corruption protests erupted into full view this week as Serbian protesters threw the country's legislature into chaos