The CDC has a new plan to address the health care worker burnout crisis
The program puts the pressure on health care leaders to lift some of the burdens of their employees

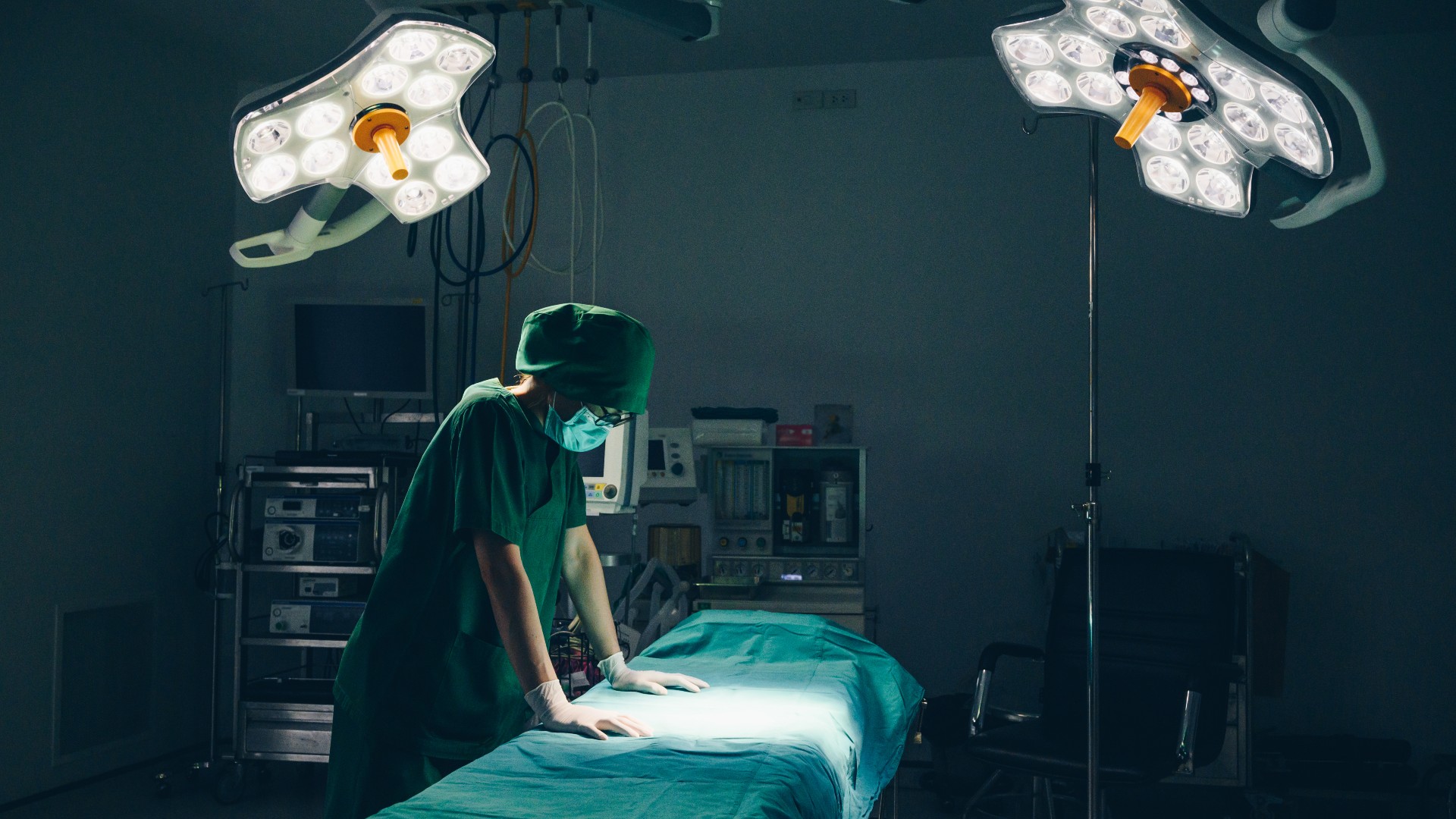
Burnout has been a persistent problem for health care workers since before the pandemic, but it is an issue that continues to plague the beleaguered industry. Too often, the responsibility of avoiding burnout is left to workers, but a new campaign from the U.S. Centers for Disease Control and Prevention (CDC) is looking to change that. The recently announced Impact Wellbeing campaign from the CDC's National Institute for Occupational Safety and Health (NIOSH) and the Dr. Lorna Breen Heroes Foundation emphasizes the need for health system leaders to step in to address the root causes of health care burnout.
Why is burnout such a pressing issue for health care workers?
The widespread burnout among health care workers is a crisis that predates the Covid-19 pandemic. But the problem has only gotten worse since then, according to a federal survey of American workers published in October by the CDC. Healthcare workers are feeling burned out more often than before the pandemic "while also struggling with symptoms of anxiety and depression, sleep problems and harassment," The New York Times summarized.
The report compared self-reported data from over a thousand adult workers tracking their mental health symptoms from 2018 to 2022. Compared to other industries, health care workers reported an uptick in the number of poor mental health days they had over a month, from 3.3 in 2018 to 4.5 in 2022. Last year, less than 30% of health care workers described themselves as very happy, also down from 2018. The findings underscored "a dire staffing crisis in the nation’s health workforce," the Times noted. The industry suffered through long hours, high turnover, increased harassment and public backlash over mask and vaccine mandates during the pandemic. In the last few years, medical employees have been leaving their jobs in droves, and others, including scores of nurses and pharmacy workers, have joined large-scale strikes.
The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
One of the things that experts say has created "widespread barriers to seeking help" is the practice of asking potential employees in high-stress environments questions about their mental health history, per Axios. Industry organizations such as the American Medical Association have pushed for the removal of these questions from applications as they might discourage physicians from seeking treatment for a mental illness or substance abuse.
"A lot of people say, 'I can't do that. I can't avail myself of that because otherwise, I'm going to lose my job,'" John Howard, director of NIOSH, told Axios.
What makes the CDC's campaign different than other efforts to alleviate burnout?
The campaign organizers noticed that too many existing initiatives focused on "resilience training," putting the responsibility on workers to cope in toxic work environments., despite evidence that fixing the environments themselves would be a better solution. The CDC survey showed that the odds of getting burned out decreased when the workers "received help from supervisors, had enough time to do their work and trusted management," the Times explained. But experts said the "efforts by medical institutions to address the mental health of their workers have been uneven at best," the outlet added.
The Impact Wellbeing campaign is aimed at helping hospital leaders fill in the gaps with "evidence-informed solutions to reduce healthcare worker burnout, sustain wellbeing and build a system where healthcare workers thrive," per the CDC. Providing individual support resources is a good first step but it is "critical to go beyond encouraging self-care to address the underlying factors that impact healthcare worker wellbeing," the organization added.
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
The campaign's tools include a questionnaire about workers' well-being and a guide that helps leaders facilitate conversations about their own experiences with mental health care. The program also offers online workshops on supporting work-life balance, veteran life and healthy sleep habits. It also includes a guide from the Dr. Lorna Breen Heroes’ Foundation for removing intrusive questions about mental health history from hospital credentialing applications.
Since the CDC cannot set any federal policies, there won't be any consequences if hospital leaders ignore the campaign. But J. Corey Feist, the foundation's co-founder and CEO, told Stat News that this could actually make it more efficient. The critical part of the campaign is that "it doesn’t wait for a federal law to be passed with a bunch of mandates," Feist said.
Theara Coleman has worked as a staff writer at The Week since September 2022. She frequently writes about technology, education, literature and general news. She was previously a contributing writer and assistant editor at Honeysuckle Magazine, where she covered racial politics and cannabis industry news.

