The cost of long COVID
The mysterious constellation of pervasive symptoms has struck millions, and no one can say how long they’ll last
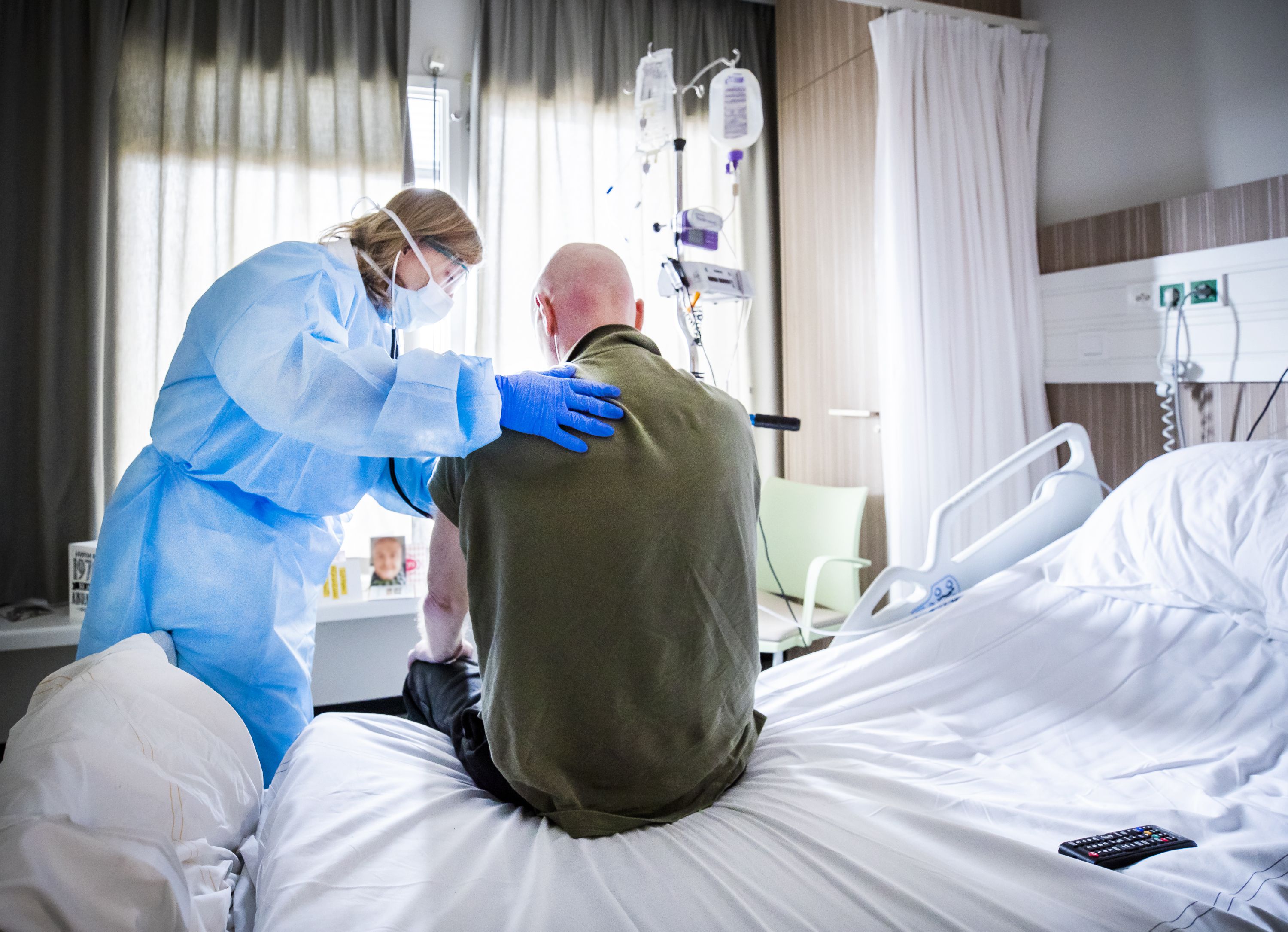
The mysterious constellation of pervasive symptoms has struck millions, and no one can say how long they'll last. Here's everything you need to know:
How many people are affected?
The CDC and states do not track long COVID cases, so there are no hard numbers, but numerous studies indicate the problem runs deep and wide. A University of Washington study found 30 percent of people who had COVID were still experiencing symptoms after six months; a study by Imperial College London showed almost 15 percent reported three or more symptoms after 12 weeks. Early research indicates between 10 and 30 percent of people who get COVID-19 may face long-term issues. More than 42 million Americans are known to have tested positive for COVID, and the real total is undoubtedly much higher. So even at the low-end estimate of 10 percent, that means millions of people in the U.S. and the world are "long-haulers," facing chronic symptoms that can impair their ability to work, exercise, or lead a normal life. Doctors who treat long COVID patients say the costs of both of their future care and lost productivity could be staggering. "I don't think anyone truly understands the magnitude of this," said Denyse Lutchmansingh, who oversees the Post-COVID-19 Recovery Program at Yale–New Haven Hospital. "The majority of my patients are in the prime of their work lives, and they're debilitated."
Subscribe to The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
What are the symptoms of long COVID?
Literally hundreds of symptoms have been reported. Among the most common are nerve and muscle pain, persistent fatigue, breathing difficulties, heart palpitations, loss of smell and taste, and gastrointestinal distress. Issues plaguing post-COVID patients range from impaired metabolic function and kidney damage to blood-clotting problems and menstrual changes. The virus "can affect nearly every organ system," said Ziyad Al-Aly, who studies long-haul patients in the Department of Veterans Affairs health system. Then there are neurological symptoms, which can be the most debilitating. They include sleep disorders, dizziness, numbness in limbs, anxiety, and brain fog marked by confusion, memory loss, and inability to concentrate. The worst cases "really look like dementia," said Jördis Frommhold, leader of a German study of long COVID, who cites patients as young as 18 who "can't form sentences." Cassandra Hernandez, a 38-year-old nurse in San Antonio, went from working on her master's degree to forgetting "how to use a fork" and struggling to read at a fifth-grade level. "It's embarrassing," she said.
What causes these problems?
There are several leading theories. One is that they're caused by fragments or reserves of the virus that linger in the body. Another possible cause is persistent inflammation or damage wrought by the initial infection, affecting blood vessels, nerve pathways, or other areas of the body. The dominant theory is that long COVID is an autoimmune disease triggered by infection by an unfamiliar virus, in which victims' revved-up immune systems continue to attack healthy tissue after the initial infection is gone. Or it could be a combination of these factors. Whatever the cause, long COVID mirrors other mysterious, chronic illnesses triggered by viral and bacterial infections. Among them is myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS), cases of which have been linked to outbreaks of SARS, Ebola, and other viruses. There are no known markers for who will develop long COVID, which affects many people with no previous health issues — and many whose initial infections were mild or asymptomatic.
Do long COVID patients improve?
The range is broad. Some patients largely return to their old selves within three or four months. Many show meaningful improvement but have lingering issues. But some remain significantly impaired after a year or more, and struggle to hold jobs. "A lot of us can't afford our medications or groceries, and quite a few of us are going homeless," said Amanda Finley, a Kansas City archaeologist who founded a Facebook discussion group for long-haulers after suffering persistent symptoms including brain fog, heart palpitations, fatigue, and shortness of breath. Treatment generally involves managing symptoms through physical therapy, cognitive exercises, and other treatments. "It's a long process, and people need to make a lot of behavioral and life adjustments," said David Putrino, a rehabilitation specialist who treats long COVID patients at New York's Mount Sinai Hospital.
What can be done?
In February, the National Institutes of Health launched a $1.2 billion initiative to study the causes and treatment of long COVID. The American Medical Association and CDC have launched initiatives to educate doctors about identifying and treating the disorder. And across the country, hospitals have established dozens of integrated clinics dedicated to long COVID, where specialists in various areas are studying the syndrome and refining treatments. "Our clinical model is constantly evolving as we learn more from our patients," said Yale's Lutchmansingh. Experts warn that we've only begun to reckon with the social and financial costs. "We're going to need resources for many years to come to deal with these patients," said Putrino.
Long COVID and the vaccinated
Do vaccines affect the odds of developing long COVID? Evidence is emerging that vaccination significantly reduces the chances of lingering symptoms, but that some vaccinated people who get breakthrough infections do in fact become long-haulers. In a small Israeli study, 19 percent of people with breakthrough infections had continuing symptoms at six weeks, and long COVID clinics in the U.S. say that some of their newer cases are vaccinated people. It's still unclear to researchers how vaccination affects these lingering symptoms; are they milder, and will they resolve more quickly? Some doctors believe that by lessening the severity of infection, vaccines will lower the odds of long COVID — and a new British study of 1.2 million adults found fully vaccinated people cut in half their odds of having symptoms four weeks after falling ill. Some experts predict the prevalence of long COVID will fall as our immune systems become increasingly familiar with the virus through vaccinations, boosters, and natural exposures. But Zijian Chen, medical director of Mount Sinai's Center for Post-COVID Care, says this is only an educated guess. "It's too early to tell," he said.
This article was first published in the latest issue of The Week magazine. If you want to read more like it, you can try six risk-free issues of the magazine here.
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
-
 July 13 editorial cartoons
July 13 editorial cartoonsCartoons Sunday's political cartoons include new TSA rules, FEMA cuts, and Volodymyr Zelenskyy complimenting Donald Trump's new wardrobe
-
 5 weather-beaten cartoons about the Texas floods
5 weather-beaten cartoons about the Texas floodsCartoons Artists take on funding cuts, politicizing tragedy, and more
-
 What has the Dalai Lama achieved?
What has the Dalai Lama achieved?The Explainer Tibet’s exiled spiritual leader has just turned 90, and he has been clarifying his reincarnation plans
-
 RFK Jr. scraps Covid shots for pregnant women, kids
RFK Jr. scraps Covid shots for pregnant women, kidsSpeed Read The Health Secretary announced a policy change without informing CDC officials
-
 New FDA chiefs limit Covid-19 shots to elderly, sick
New FDA chiefs limit Covid-19 shots to elderly, sickspeed read The FDA set stricter approval standards for booster shots
-
 RFK Jr.: A new plan for sabotaging vaccines
RFK Jr.: A new plan for sabotaging vaccinesFeature The Health Secretary announced changes to vaccine testing and asks Americans to 'do your own research'
-
 Five years on: How Covid changed everything
Five years on: How Covid changed everythingFeature We seem to have collectively forgotten Covid’s horrors, but they have completely reshaped politics
-
 HMPV is spreading in China but there's no need to worry
HMPV is spreading in China but there's no need to worryThe Explainer Respiratory illness is common in winter
-
 Marty Makary: the medical contrarian who will lead the FDA
Marty Makary: the medical contrarian who will lead the FDAIn the Spotlight What Johns Hopkins surgeon and commentator Marty Makary will bring to the FDA
-
 Long Covid: study shows damage to brain's 'control centre'
Long Covid: study shows damage to brain's 'control centre'The Explainer Research could help scientists understand long-term effects of Covid-19 as well as conditions such as MS and dementia
-
 FDA OKs new Covid vaccine, available soon
FDA OKs new Covid vaccine, available soonSpeed read The CDC recommends the new booster to combat the widely-circulating KP.2 strain